62nd National Congress of the Italian Society of Rheumatology
Vol. 77 No. s1 (2025): Abstract book of the 62th Conference of the Italian Society for...
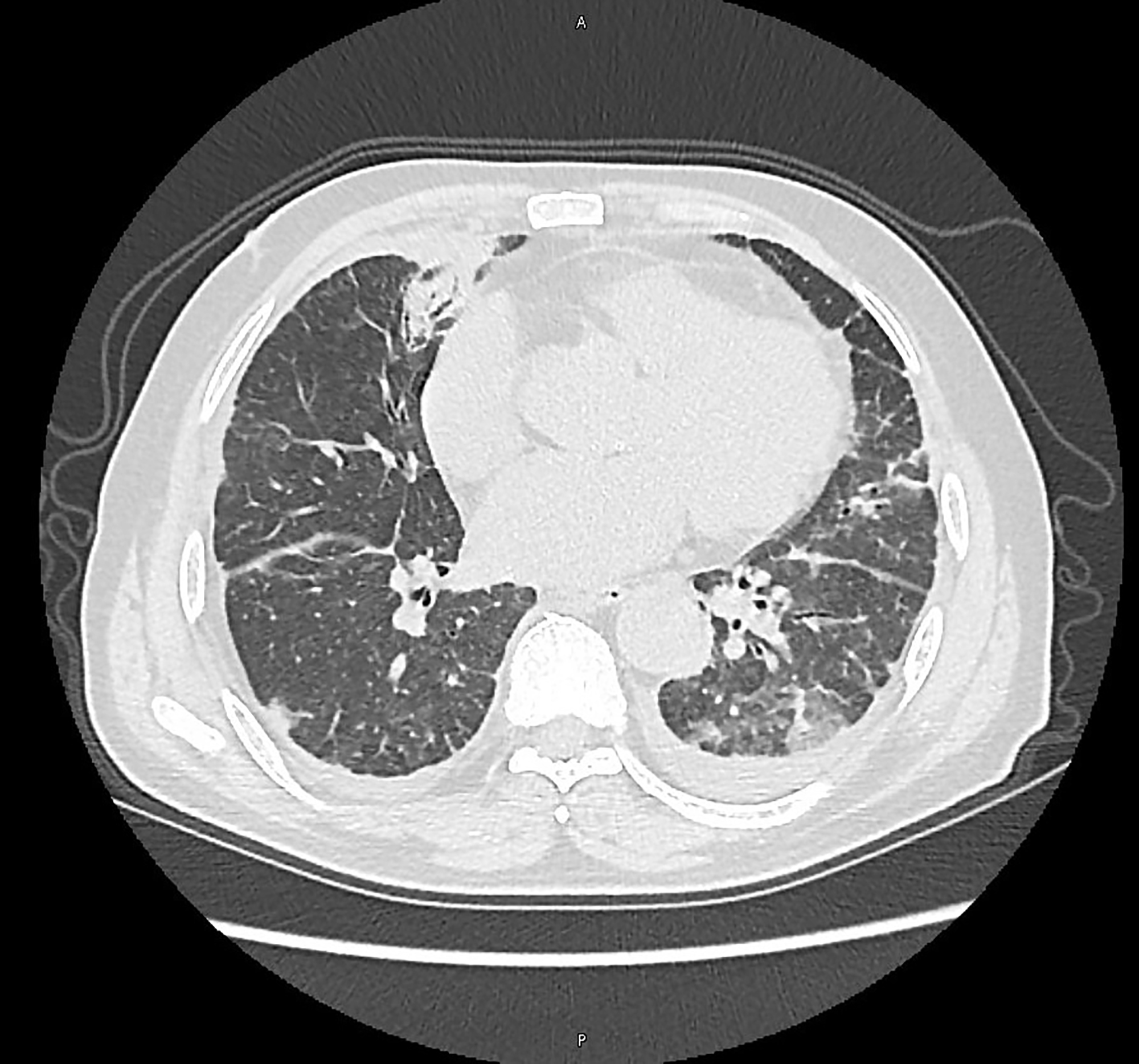
PO:22:038 | Recurrent Pneumonias and Persistent Inflammation in VEXAS Syndrome: The Role of BAL in Differential Diagnosis
Francesco Ghellere1, Bernardo D'Onofrio1, Maria Chiara Ditto1, Salvatore Panaro1, Francesca Piccione1|2, Giacomo Tanti1, Enrico Fusaro1, Simone Parisi1 | 1SC Reumatologia, Città della Salute e della Scienza Torino, Italy; 2Fondazione Ricerca Molinette Torino, Italy
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 18 March 2026
37
Views