62nd National Congress of the Italian Society of Rheumatology
Vol. 77 No. s1 (2025): Abstract book of the 62th Conference of the Italian Society for...
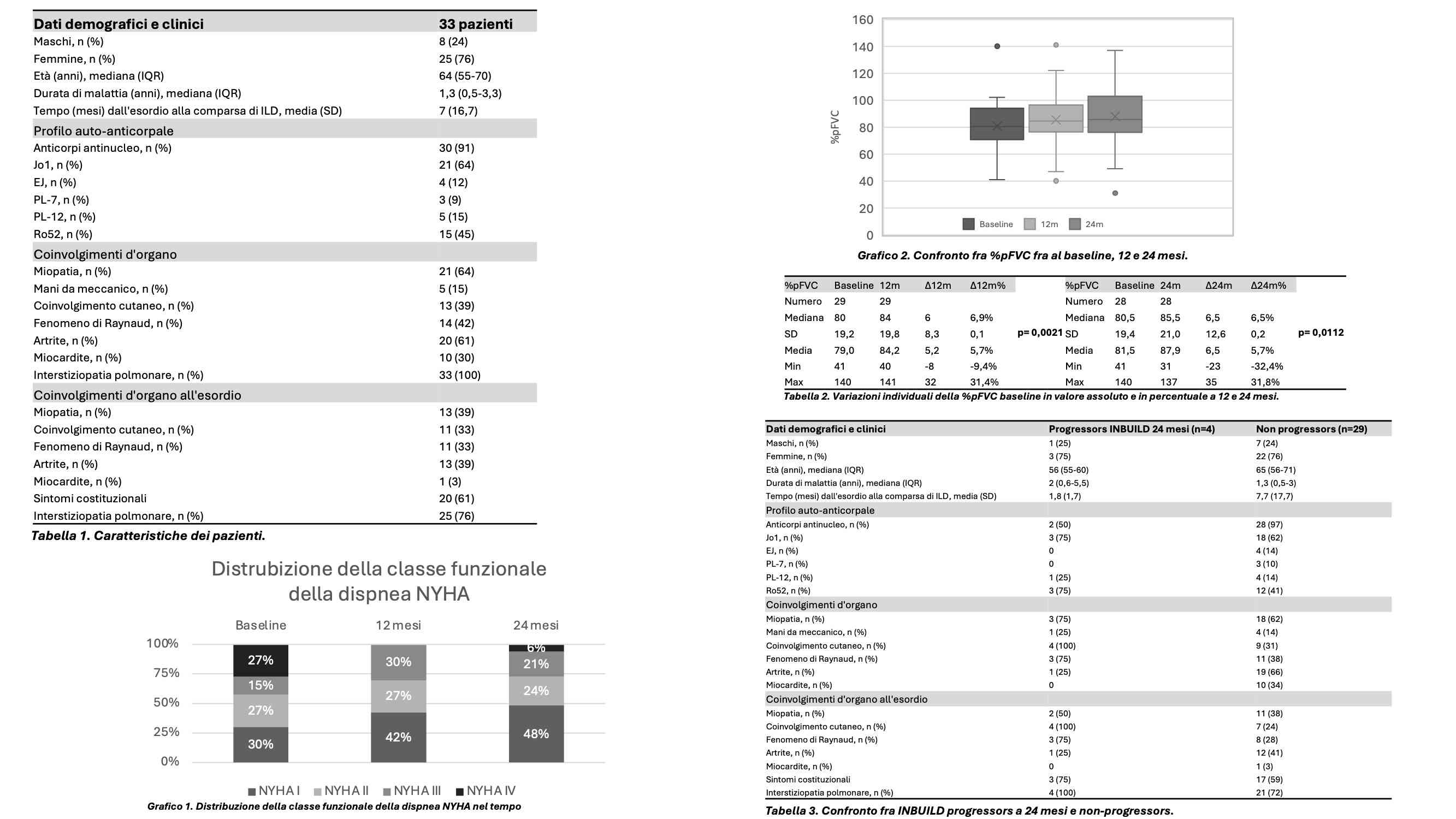
PO:25:073 | Pulmonary involvement and progressive interstitial lung disease in anti-synthetase syndrome: a single-center retrospective study
Daniele Scaramuzzi1|3, Giacomo De Luca1|3, Veronica Batani1, Giulia Buonsante1|3, Lorenzo Dagna1|3, Marco Matucci-Cerinic1|2|3, Corrado Campochiaro1|2|3 | 1Unità di Immunologia, Reumatologia, Allergologia e Malattie Rare, IRCCS Ospedale San Raffaele, Milano; 2Inflammation, Fibrosis and Ageing Initiative INFLAGE, IRCCS San Raffaele Hospital, Milano; 3Università Vita-Salute San Raffaele, Milano, Italy
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 25 November 2025
170
Views