62nd National Congress of the Italian Society of Rheumatology
Vol. 77 No. s1 (2025): Abstract book of the 62th Conference of the Italian Society for...
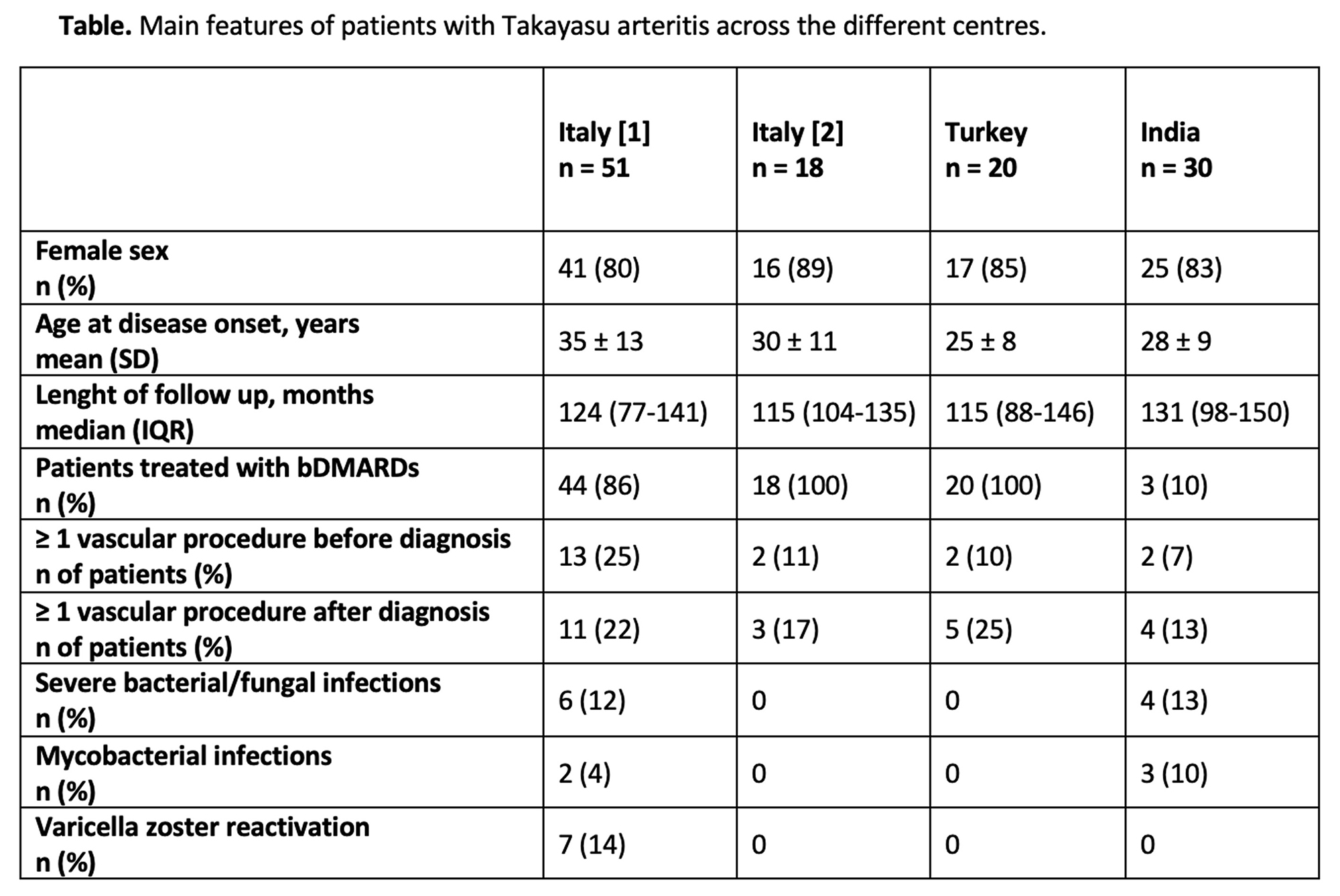
PO:36:252 | Long-Term Outcomes of Patients with Takayasu Arteritis in the Era of Biological Agents: a Multicenter International Study
Alessandro Tomelleri1, Durga Prasanna Misra2, Fatma Alibaz-Oner3, Chiara Marvisi4, Chiara Calabrese1, Upendra Rathore2, Aysegul Avcu3, Adele Del Giudice4, Elisabetta Olivi4, Caterina Ricordi4, Corrado Campochiaro1, Elena Baldissera1, Marco Matucci-Cerinic1, Haner Direskeneli3, Carlo Salvarani4, Lorenzo Dagna1 | 1IRCCS Ospedale San Raffaele, Unità di Immunologia, Reumatologia, Allergologia e Malattie Rare Milano, Italy; 2Sanjay Gandhi Postgraduate Institute of Medical Sciences SGPGIMS, Clinical Immunology and Rheumatology Lucknow Country, India; 3Marmara University, School of Medicine, Department of Internal Medicine, Division of Rheumatology Istanbul, Turkey; 4Azienda USL-IRCCS di Reggio Emilia, Unità di Reumatologia Reggio Emilia, Italy
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 18 March 2026
28
Views