62nd National Congress of the Italian Society of Rheumatology
Vol. 77 No. s1 (2025): Abstract book of the 62th Conference of the Italian Society for...
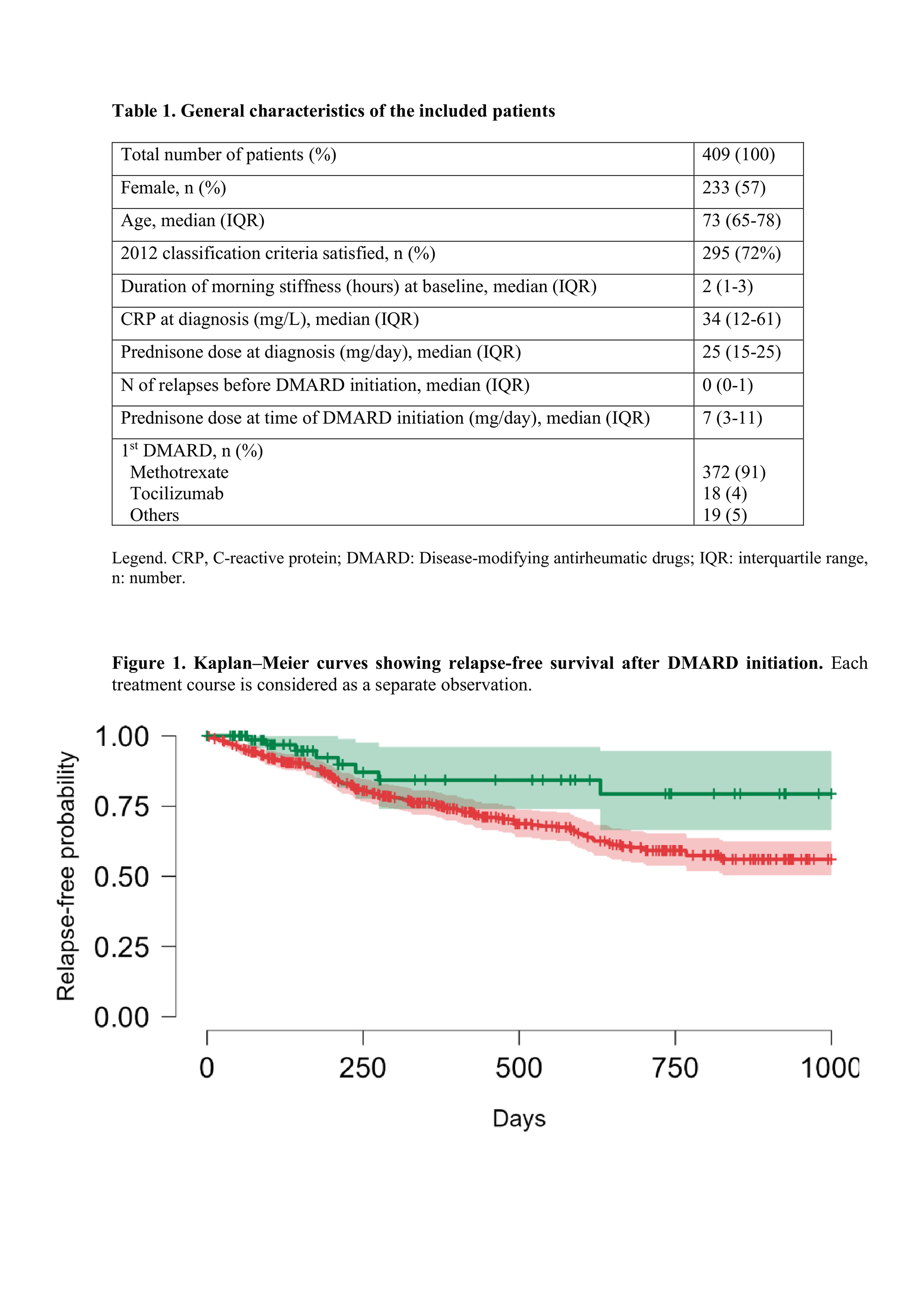
PO:35:233 | Tocilizumab is associated with improved relapse-free survival in polymyalgia rheumatica: a multicentre retrospective study
Milena Bond1, Giovanni Adami2, Marianna Tamussin3, Mario Frasca4, Sara Zandonella Callegher1, Marcello Govoni3, Maurizio Rossini2, Lorenzo Dagna4, Marco Matucci Cerinic4, Christian Dejaco1, Alessandro Tomelleri4 | 1Department of Rheumatology, Brunico Hospital ASAA-SABES, Teaching Hospital of the Paracelsius Medical University Bunico, Italy; 2Rheumatology Unit, University of Verona, Policlinico Borgo Roma Verona, Italy; 3Rheumatology Unit, Department of Medical Sciences, University of Ferrara and Azienda Ospedaliero-Universitaria S. Anna Ferrara, Italy; 4Unit of Immunology, Rheumatology, Allergy and Rare Diseases, IRCCS San Raffaele Hospital Milano, Italy
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 18 March 2026
25
Views