62nd National Congress of the Italian Society of Rheumatology
Vol. 77 No. s1 (2025): Abstract book of the 62th Conference of the Italian Society for...
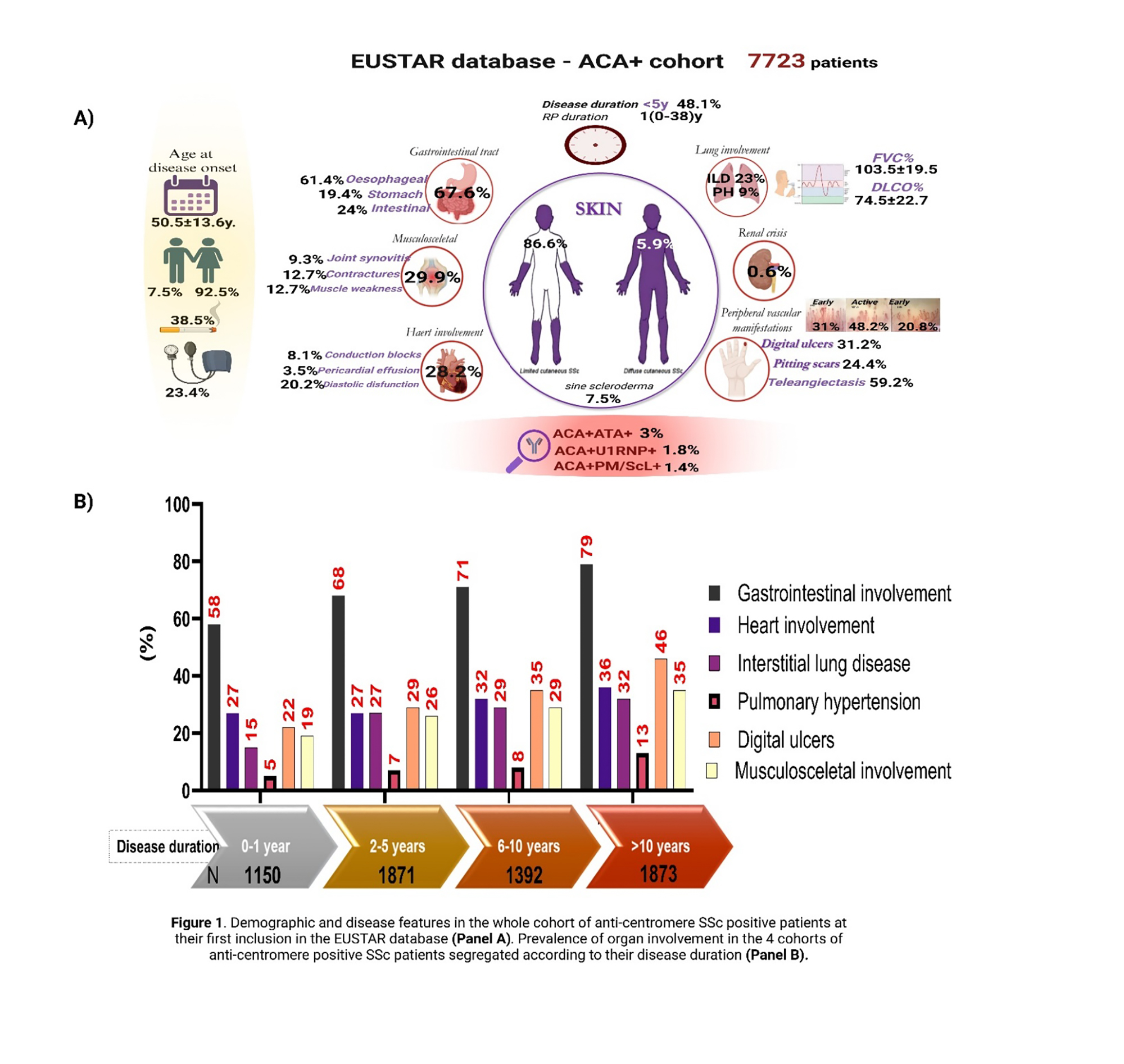
PO:32:182 | Disease characteristics of anti-centromere positive systemic sclerosis patients and risk factors for organ involvement: data from the EUSTAR cohort
Corrado Campochiaro1, Jelena Colic2, Del Papa Nicoletta3, Oliver Distler4, Serena Guiducci5, Florenzo Iannone6, David Launay7, Yair Levy8, Britta Maurer9, Arsene Mekinian10, Predrag Ostojic2, Gabriela Riemekasten11, Petros Sfikakis12, Bojana Stamenkov13, Ulrich Walker14, Marie Elise Truchetet15, Madelon Vonk16, Francesco Del Galdo17, Giacomo De Luca1, Lorenzo Dagna1, Marco Matucci Cerinic1, Yannick Allanore18 | 1IRCCS San Raffaele Hospital; Vita Salute San Raffaele University Milan, Italy; 2University of Belgrade Belgrade, Serbia; 3UOC Reumatologia Clinica, ASST G. Pini CTO Milan, Italy; 4University Hospital Zurich Zurich, Switzerland; 5Department of Rheumatology, University of Florence Florence, Italy; 6Rheumatology Unit Bari, Italy; 7CHU Lille Lille, France; 8Department of Medicine Kfar Saba, Israel; 9Department for BioMedical Research, University of Bern Bern, Switzerland; 10Service de medecine interne Paris, France; 11Department of Rheumatology University of Lubeck Lubeck Germany; 12National and Kapodistrian University of Athens Athens, Greece; 13University School of Medicine, Nis Nis, Serbia; 14University Hospital Basel, Basel Basel, Switzerland; 15Bordeaux Hospital and University Bordeaux, France; 16Radboud University Nijmegen Medical Centre, Nijmegen, The Netherlands; 17Leeds Institute of Rheumatic and Muskuloskeletal Medicine Leeds, United Kingdom; 18Cochin Hospital Paris, France
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 18 March 2026
29
Views
Corrado Campochiaro, Jelena Colic, Del Papa Nicoletta, Oliver Distler, Serena Guiducci, Florenzo Iannone, David Launay, Yair Levy, Britta Maurer, Arsene Mekinian, Predrag Ostojic, Gabriela Riemekasten, Petros Sfikakis, Bojana Stamenkov, Ulrich Walker, Marie Elise Truchetet, Madelon Vonk, Francesco Del Galdo, Giacomo De Luca, Lorenzo Dagna, Marco Matucci Cerinic, Yannick Allanore