62nd National Congress of the Italian Society of Rheumatology
Vol. 77 No. s1 (2025): Abstract book of the 62th Conference of the Italian Society for...
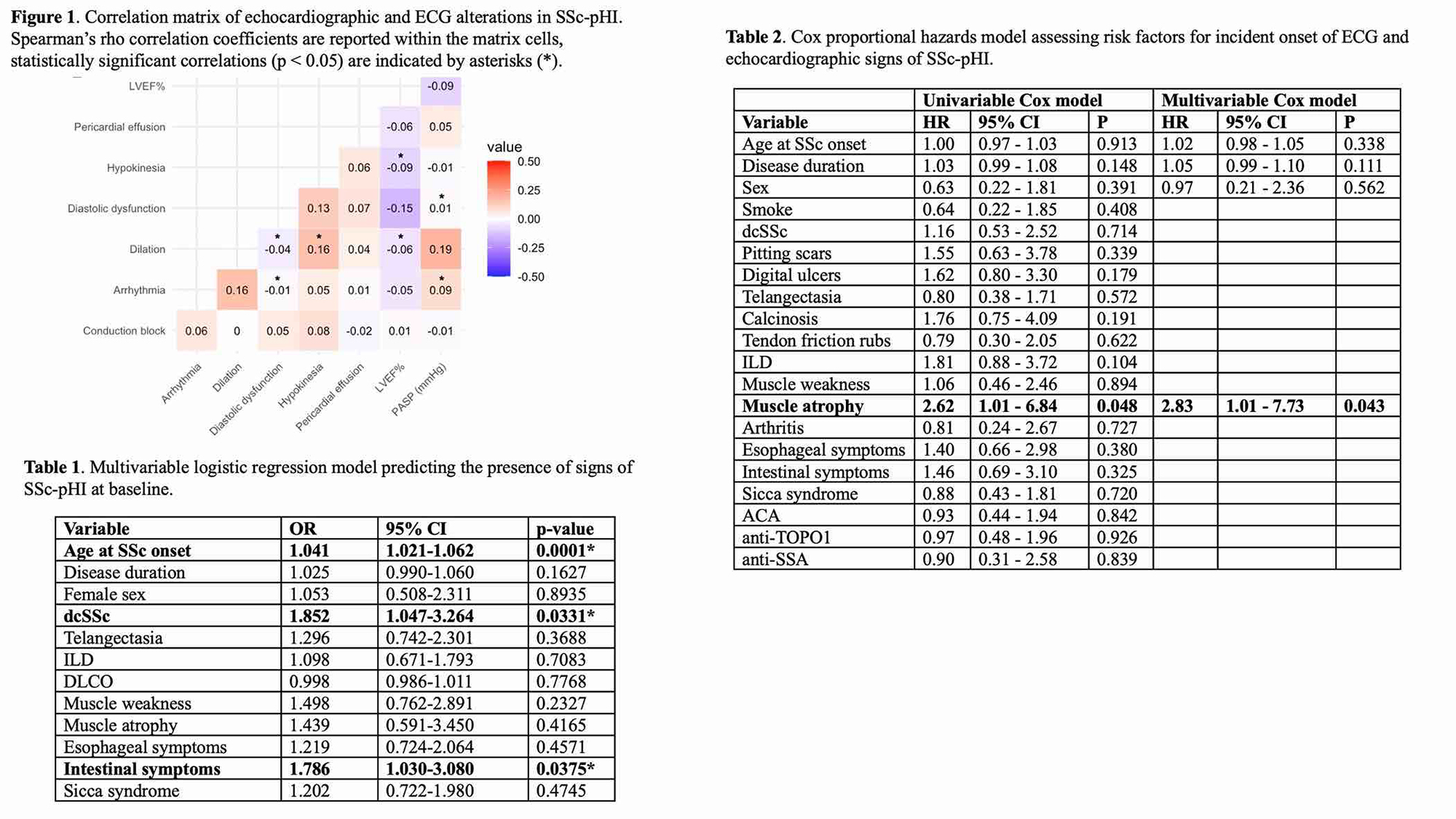
PO:31:161 | First-line diagnostic tests to intercept primary heart involvement in systemic sclerosis: clinical associations from the SPRING-SIR registry
Antonio Tonutti1|2, Francesca Motta1|2, Rossella De Angelis3, Valeria Riccieri4, Silvia Laura Bosello5, Fabio Cacciapaglia6, Veronica Codullo7, Giacomo De Luca8, Francesca Ingegnoli9, Dilia Giuggioli10, Clodoveo Ferri10, Marco Matucci-Cerinic8, Carlo Selmi1|2, Maria De Santis1|2 | 1Department of Biomedical Sciences, Humanitas University Pieve Emanuele, Milan, Italy; 2Rheumatology and Clinical Immunology, IRCCS Humanitas Research Hospital Rozzano, Milan, Italy; 3Università Politecnica delle Marche Ancona, Italy; 4Università degli Studi di Roma La Sapienza Roma, Italy; 5Università Cattolica del Sacro Cuore Roma, Italy; 6Università degli Studi di Bari Aldo Moro Bari, Italy; 7Reumatologia, Fondazione IRCCS Policlinico San Matteo Pavia, Italy; 8Università Vita-Salute San Raffaele Milano, Italy; 9Università degli Studi di Milano, Italy; 10Università degli Studi di Modena e Reggio Emilia, Italy
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 18 March 2026
26
Views