62nd National Congress of the Italian Society of Rheumatology
Vol. 77 No. s1 (2025): Abstract book of the 62th Conference of the Italian Society for...
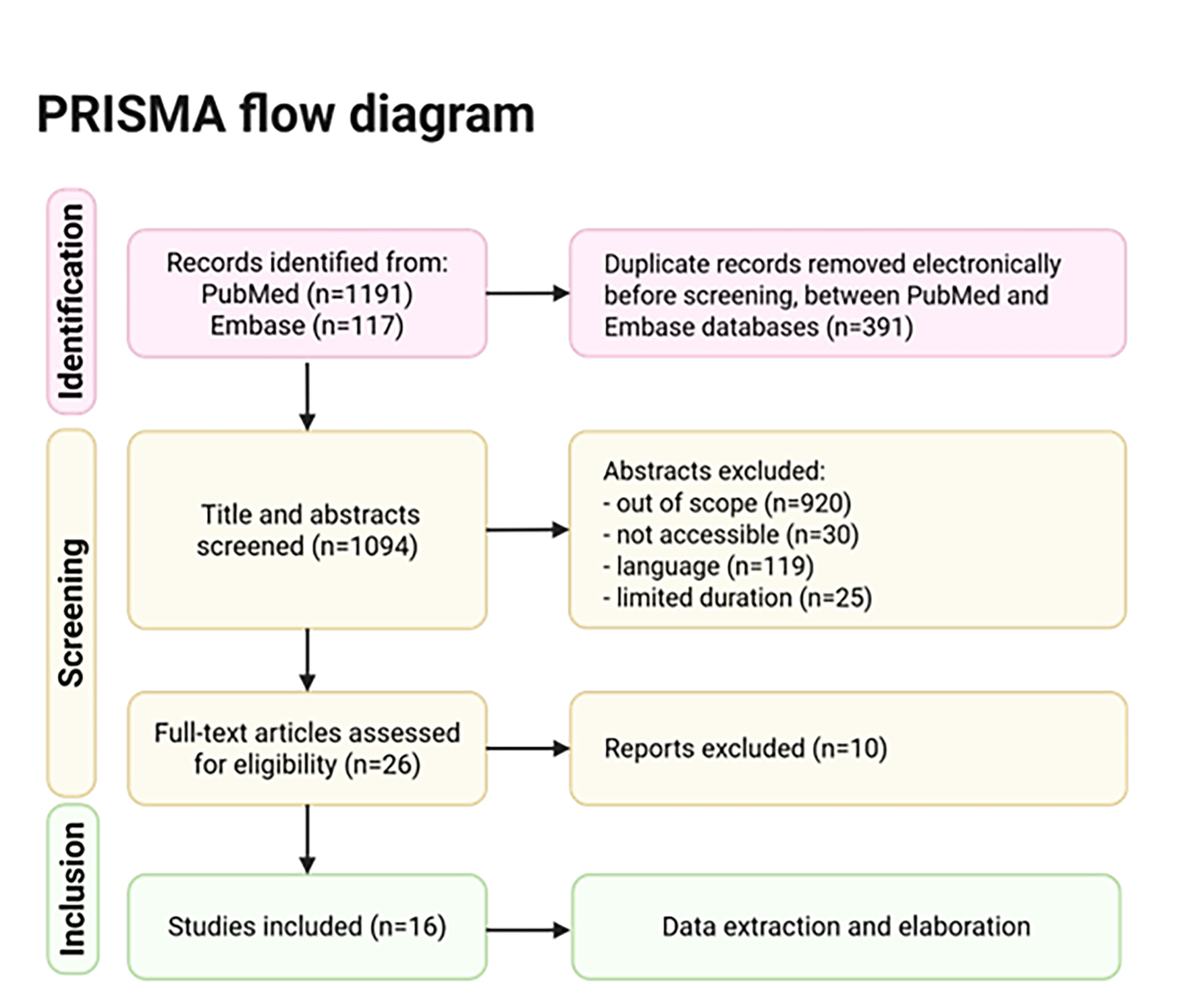
PO:30:153 | Long-term outcomes of JIA-associated uveitis: a systematic review and meta-analysis
Laura Scagnellato1, Giacomo Cozzi1, Matteo Molfese1, Mariagrazia Lorenzin1, Jamie Alexander King1, Gianluca Poncina1, Stefano Rizzetto1, Roberta Ramonda1 | 1UOC Reumatologia, Dipartimento di Medicina dei Sistemi DIMED, Ospedale Università di Padova, Italy
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 18 March 2026
51
Views