62nd National Congress of the Italian Society of Rheumatology
Vol. 77 No. s1 (2025): Abstract book of the 62th Conference of the Italian Society for...
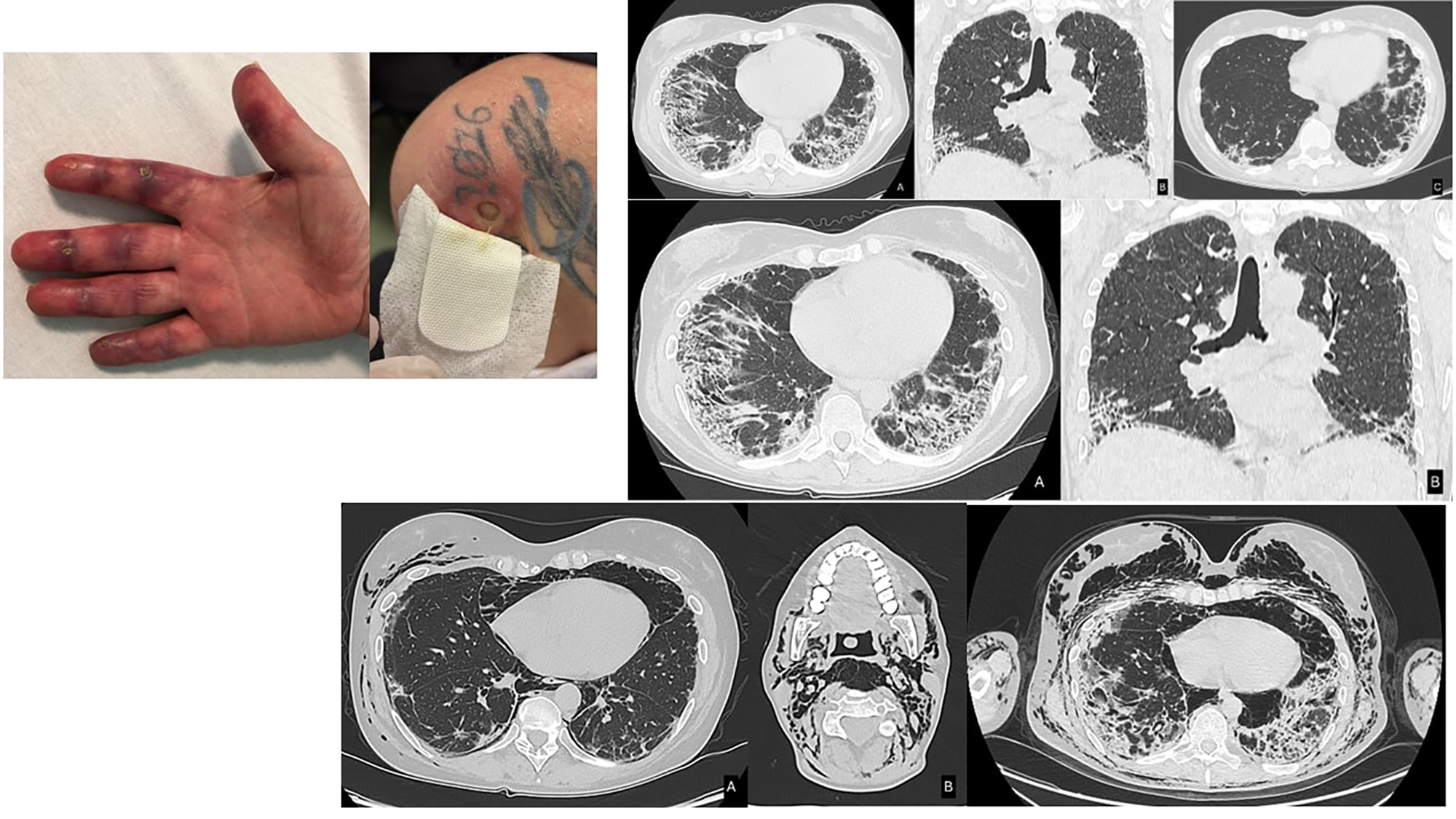
PO:24:068 | Case Report: ‘Spontaneous Pneumomediastinum in a Patient with MDA5-Positive Dermatomyositis and Severe Pulmonary Fibrosis’
Carlotta Braga1, Margherita Rizzo1, Marta Raschellà1, Beatrice Maranini1, Gioacchino Schifino2, Aldo Carnevale3, Marcello Govoni1, Andrea Lo Monaco1 | 1Rheumatology Unit, Department of Medical Sciences, University of Ferrara and Azienda Ospedaliero-Universitaria S. Anna Ferrara, Italy; 2Respiratory Medicine Unit, Department of Cardio-Thoracic-Vascular Pathologies, Arcispedale Sant'Anna, Ferrara, Italy; 3Radiology Unit, Department of Translational Medicine, University of Ferrara, Italy
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 18 March 2026
30
Views