62nd National Congress of the Italian Society of Rheumatology
Vol. 77 No. s1 (2025): Abstract book of the 62th Conference of the Italian Society for...
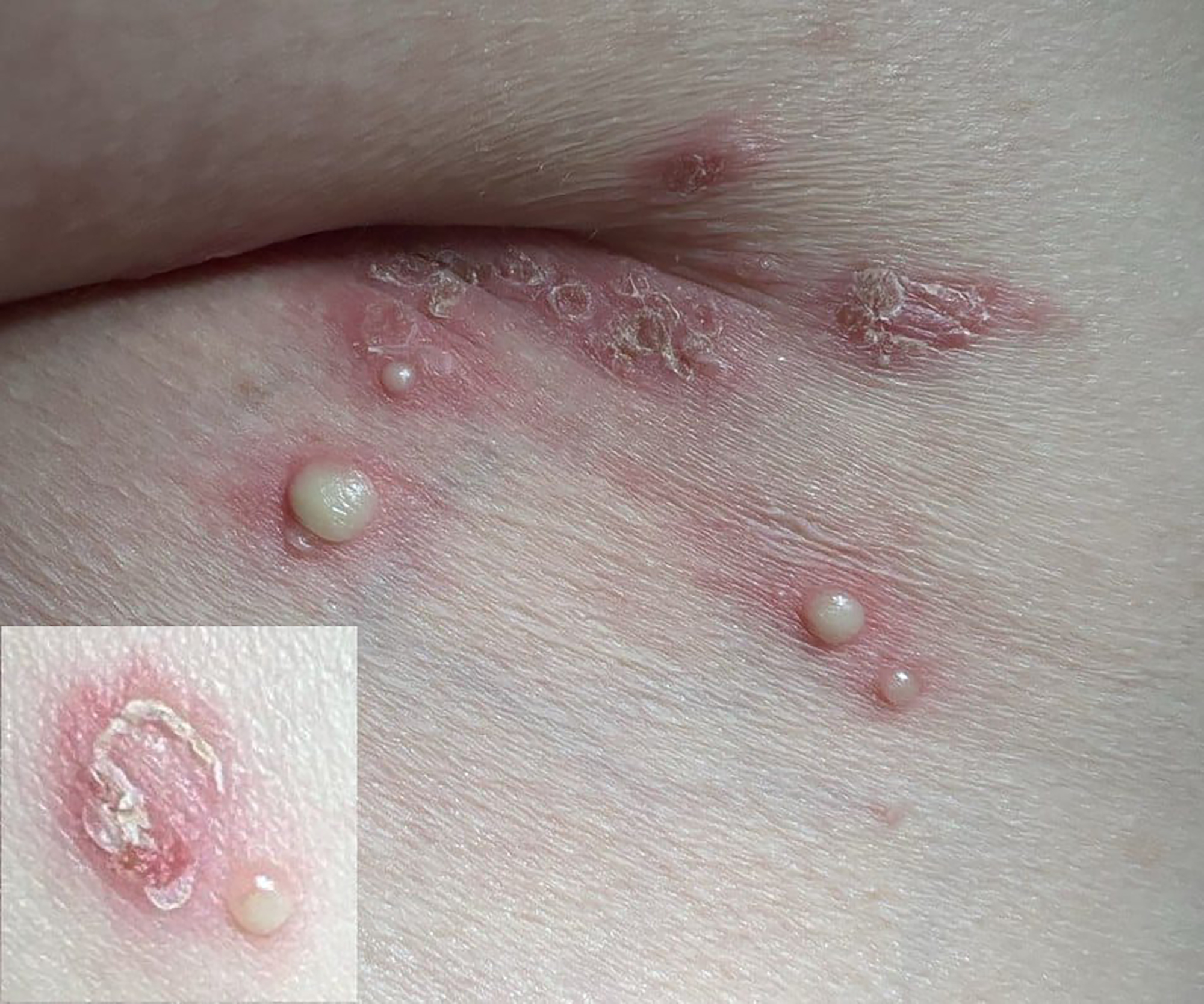
PO:22:032 | Beyond the joints: a rare case of subcorneal pustular dermatosis in Rheumatoid Arthritis
Sara Casella1|2, Carlo Smirne1|2, Roberta Zaira Pedrazzoli3, Mattia Perazzi1|3, Edoardo Cammarata4, Francesca Zottarelli4, Paola Savoia5, Renzo Boldorini6, Mario Pirisi1|2, Pier Paolo Sainaghi1|3 | 1Dipartimento di Medicina Traslazionale, Università del Piemonte Orientale Novara, Italy; 2Unità di Medicina Interna, Azienda Ospedaliera Maggiore della Carità Novara, Italy; 3Unità di Medicina Interna e Reumatologia, Azienda Ospedaliera Maggiore della Carità Novara, Italy; 4Unità di Dermatologia, Azienda Ospedaliera Maggiore della Carità Novara, Italy; 5Dipartimento di Scienze della salute, Università del Piemonte Orientale Novara, Italy; 6Unità di Anatomia Patologica, Azienda Ospedaliera Maggiore della Carità Novara, Italy
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 18 March 2026
43
Views