62nd National Congress of the Italian Society of Rheumatology
Vol. 77 No. s1 (2025): Abstract book of the 62th Conference of the Italian Society for...
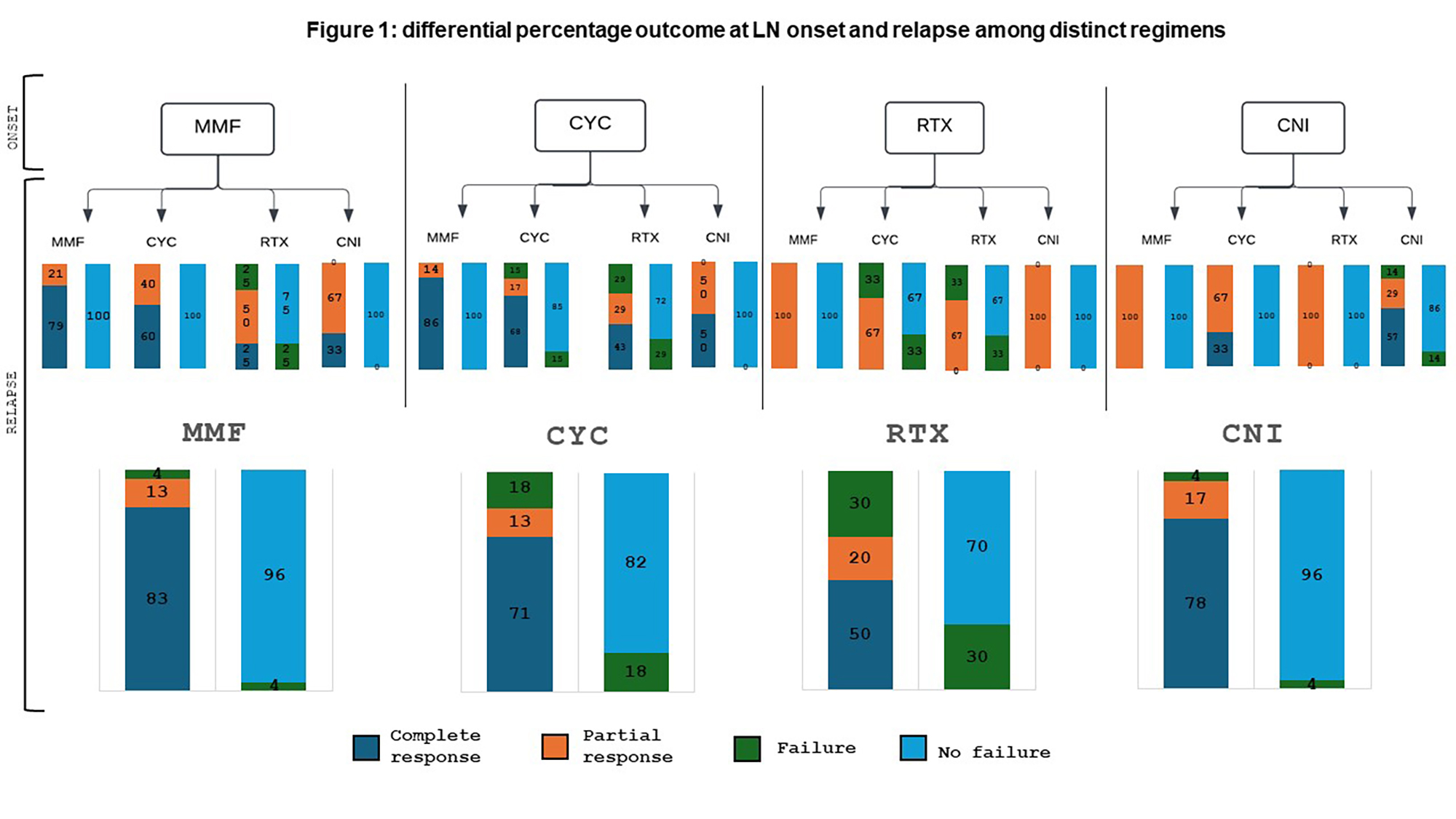
PO:16:234 | Differential efficacy of induction treatments for lupus nephritis at onset and relapses: an observational study
Giuseppe Alvise Ramirez1|2, Gabriele D Gallina1, Chiara Calabrese1|2, Serena Nannipieri1|2, Marta Calatroni3|4, Francesco Reggiani3|4, Giovanni Benanti1, Enrica Paola Bozzolo1, Raffaele Ceniccola2, Luca Moroni1|2, Marco Matucci-Cerinic1|2, Gabriella Moroni3|4, Lorenzo Dagna1|2 | 1IRCCS San Raffaele Hospital, Unit of Immunology, Rheumatology, Allergy and Rare Diseases Milan, Italy; 2Vita- Salute San Raffaele University Milan, Italy; 3IRCCS Humanitas Research Hospital, Nephrology and Dialysis Division Rozzano, Milan, Italy; 4Humanitas University, Department of Biomedical Sciences Rozzano, Milan, Italy
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 18 March 2026
44
Views