62nd National Congress of the Italian Society of Rheumatology
Vol. 77 No. s1 (2025): Abstract book of the 62th Conference of the Italian Society for...
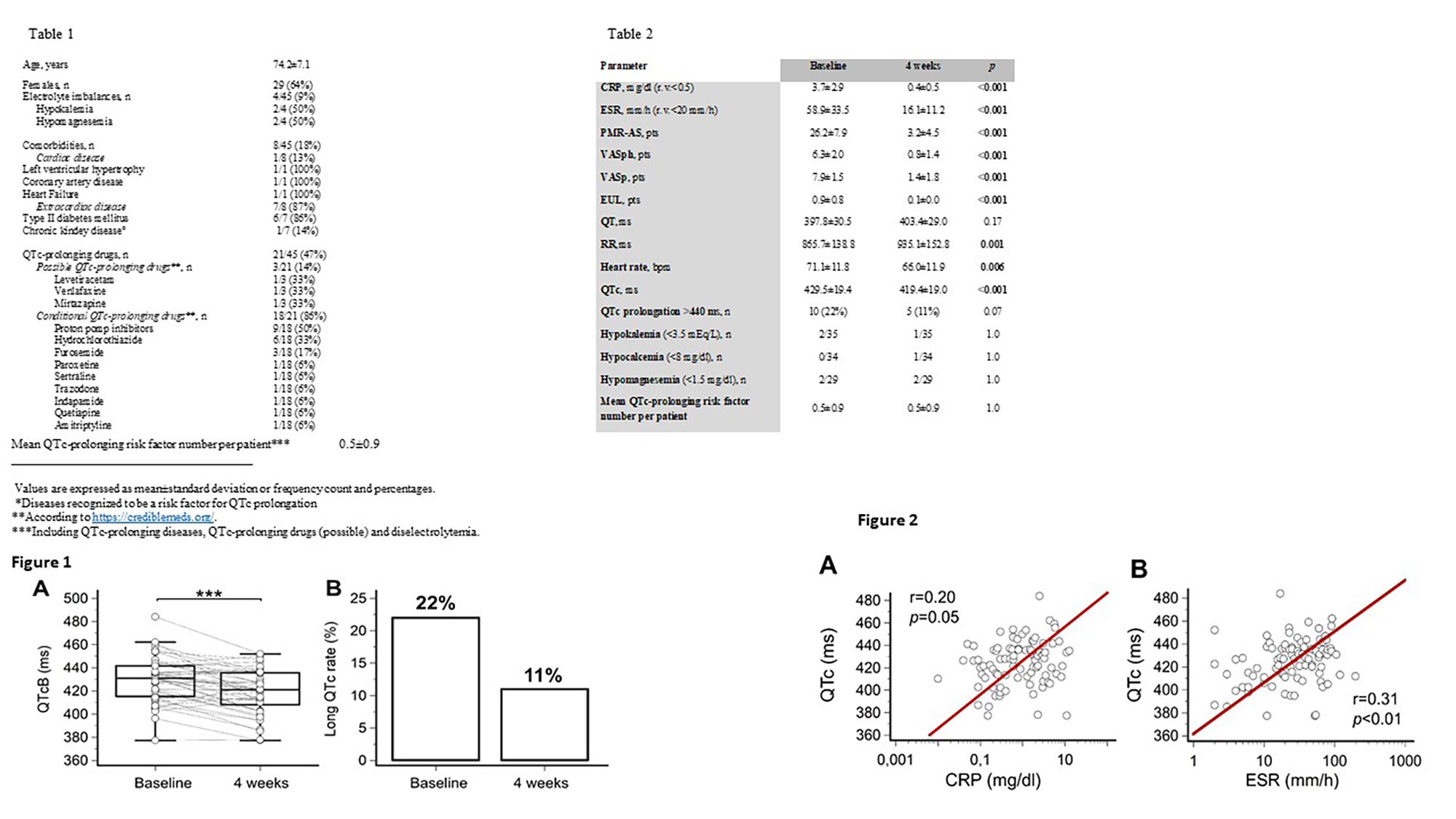
PO:12:177 | Systemic inflammation and QTc interval prolongation in new-onset polymyalgia rheumatica: the effect of corticosteroid therapy
Anna Colangelo1, Riccardo Accioli2, Viola Salvini2, Francesco Tromby1, Giulia Cruciani1, Martina Nicchi1, Biancamaria Pianese1, Francesca Lalli1, Anna Cantore2, Caterina Antonini1, Decoroso Verrengia2, Andrea Castellucci1, Giacomo Cafaro1, Carlo Perricone1, Roberto Gerli1, Pietro Enea Lazzerini2, Elena Bartoloni1 | 1SC Reumatologia. Università di Perugia, Italy; 2Dipartimento di Scienze Mediche, Università di Siena, Italy
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 18 March 2026
43
Views