62nd National Congress of the Italian Society of Rheumatology
Vol. 77 No. s1 (2025): Abstract book of the 62th Conference of the Italian Society for...
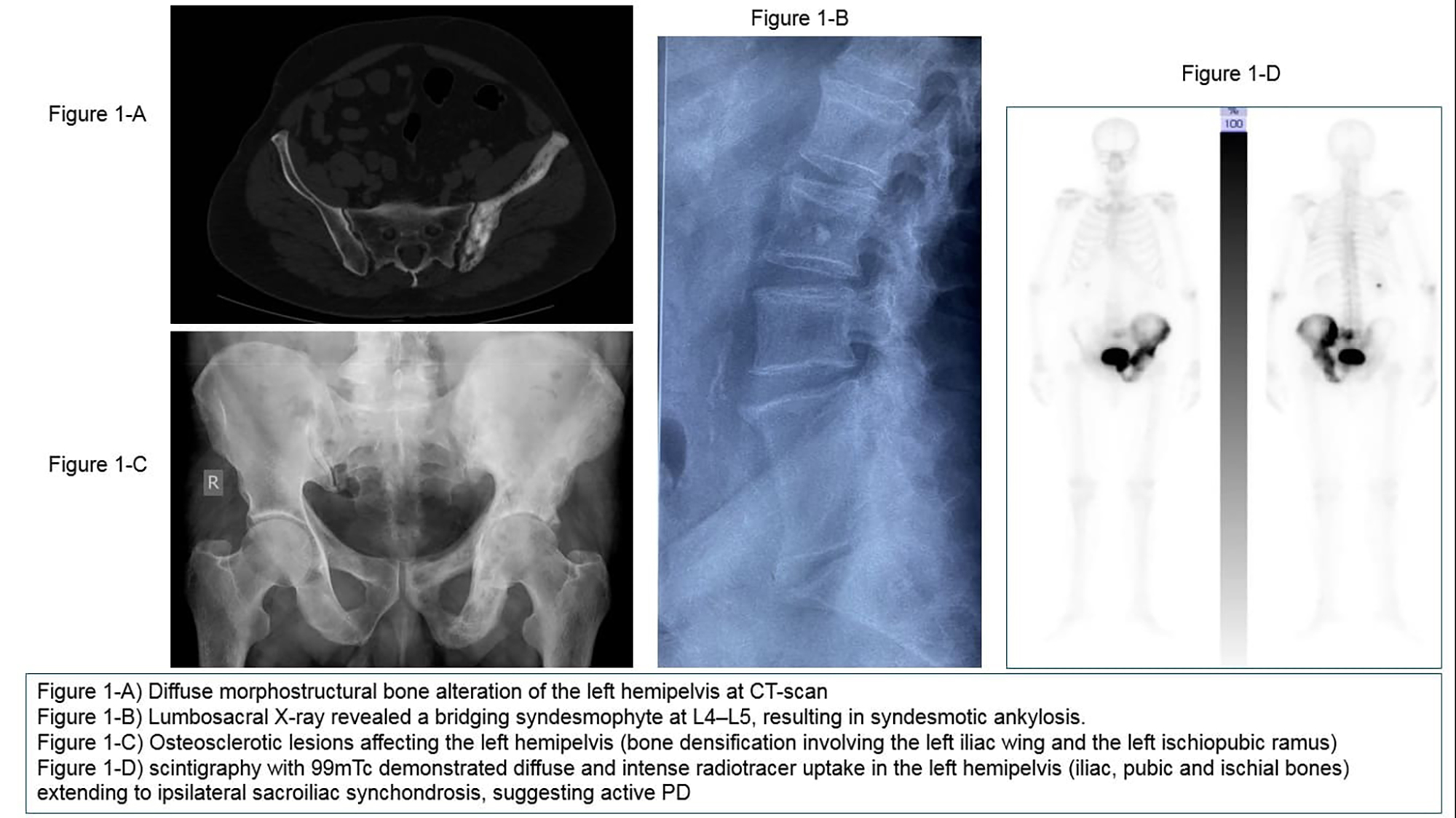
PO:11:170 | When Paget Meets Inflammatory Back Pain: A Diagnostic Dilemma Between Bone Remodeling and Spondyloarthritis
Marco Capodiferro1, Giuseppe Lopalco1, Giulia Righetti2, Gianluigi Della Corte2, Patrizia Suppressa2, Florenzo Iannone1, Fabio Cacciapaglia1|2 | 1Unit of Rheumatology, Department of Precision and Regenerative Medicine, Area Jonica DiMePRe-J, University of Bari, Italy; 2Miulli General Hospital Acquaviva - Department of Medicine and Surgery, LUM F. De Gennaro University, Casamassima, Bari, Acquaviva delle Fonti, Italy
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 18 March 2026
71
Views