62nd National Congress of the Italian Society of Rheumatology
Vol. 77 No. s1 (2025): Abstract book of the 62th Conference of the Italian Society for...
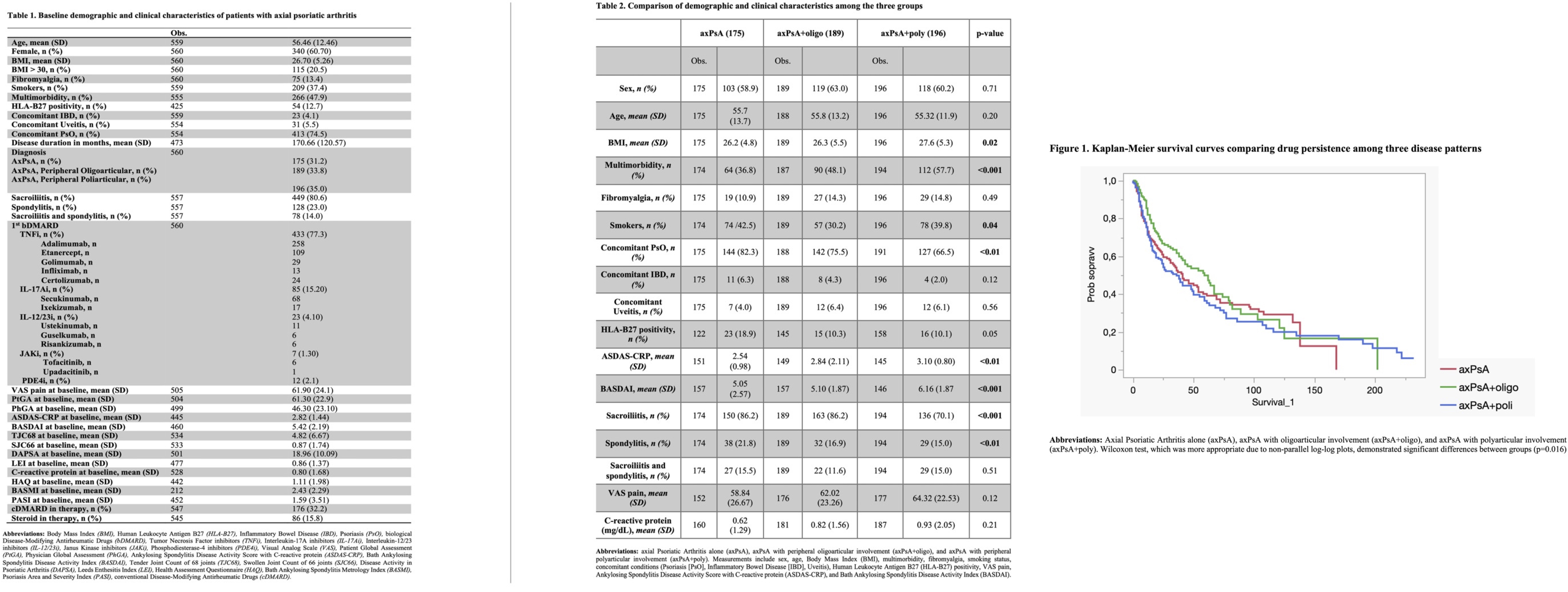
PO:03:037 | The Impact of Peripheral Joint Involvement, Pain, and Inflammatory Bowel Diseases on Drug Persistence in Axial Psoriatic Arthritis
Giuseppe Lopalco1, Sergio Del Vescovo1, Maria Sole Chimenti2, Giuliana Guggino3, Serena Guiducci4, Eleonora Celletti5, Alberto Cauli6, Luca Cantarini7, Valentino Paci8, Eneida Cela2, Lidia La Barbera3, Gemma Lepri4, Myriam Di Penta5, Alberto Floris6, Alice Agostinelli8, Vincenzo Venerito1, Michele Maria Luchetti8, Florenzo Iannone1 | 1Rheumatology Unit, Department of Precision and Regenerative Medicine and Ionian Area, Bari, Italy; 2Reumatology, Allergology and Clinical Immunology University of Rome Tor Vergata, Roma, Italy; 3Department of Health Promotion Sciences, Maternal and Infant Care, Internal Medicine and Medical Specialties, Palermo, Italy; 4Divisions of Internal Medicine and Rheumatology AOUC, Department of Experimental and Clinical Medicine, Firenze, Italy; 5Rheumatology Unit, SS. Annunziata Hospital of Chieti, G. D'Annunzio, Chieti, Italy; 6Department of Medical Science and Public Health, Cagliari, Italy; 7Policlinico Le Scotte, Siena, Italy; 8Clinical Medicine, Dipartimento di Scienze Cliniche e Molecolari, Università Politecnica delle Marche, Ancona, Italy
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 18 March 2026
19
Views
Giuseppe Lopalco, Sergio Del Vescovo, Maria Sole Chimenti, Giuliana Guggino, Serena Guiducci, Eleonora Celletti, Alberto Cauli, Luca Cantarini, Valentino Paci, Eneida Cela, Lidia La Barbera, Gemma Lepri, Myriam Di Penta, Alberto Floris, Alice Agostinelli, Vincenzo Venerito, Michele Maria Luchetti, Florenzo Iannone