62nd National Congress of the Italian Society of Rheumatology
Vol. 77 No. s1 (2025): Abstract book of the 62th Conference of the Italian Society for...
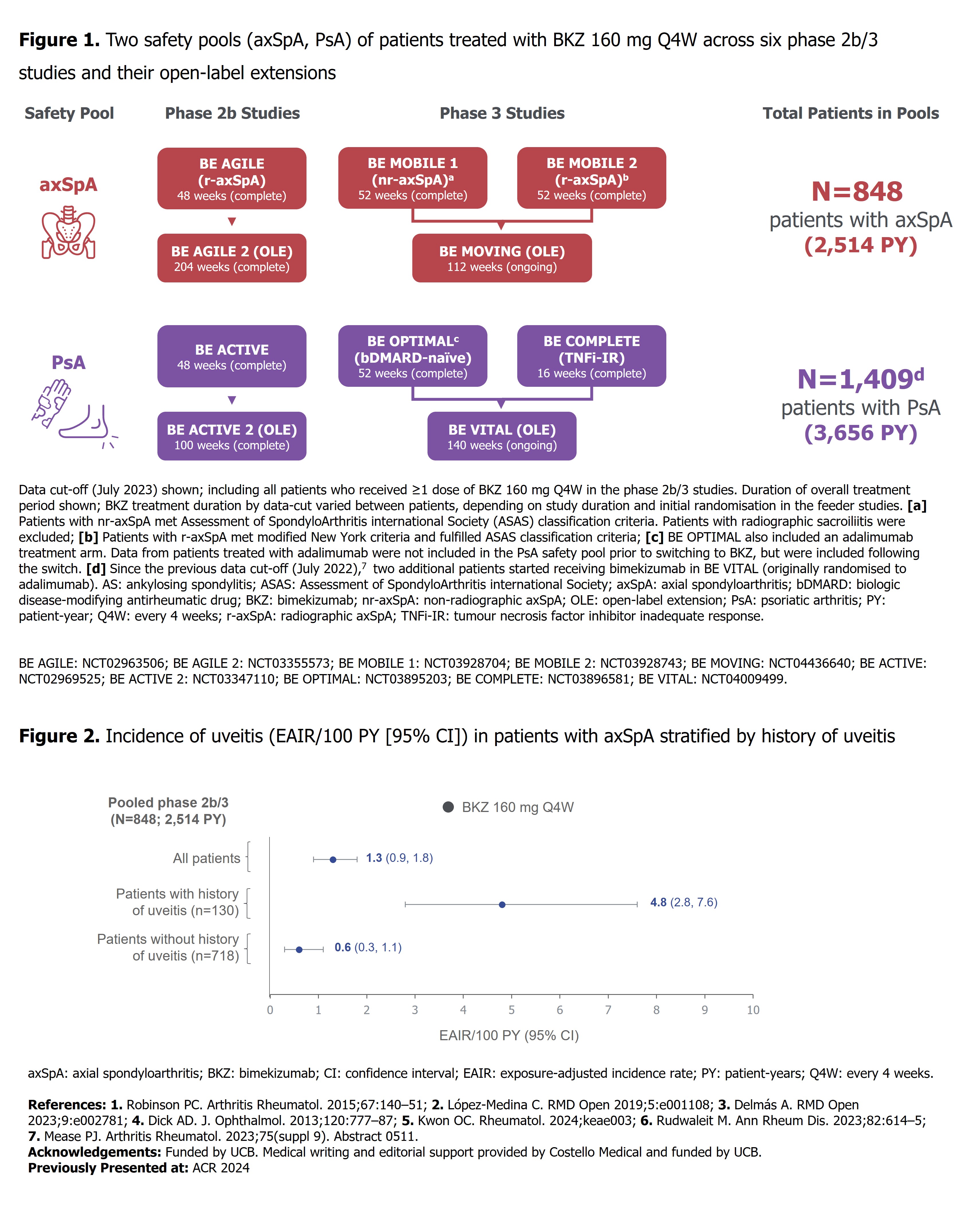
PO:03:033 | Low Uveitis Rates in Patients with Axial Spondyloarthritis or Psoriatic Arthritis Treated with Bimekizumab: Long-Term Results from Phase 2b/3 Trials
Irene E Van Der Horst-Bruinsma1, Matthew A Brown2, Floris A Van Gaalen3, Nigil Haroon4, Lianne S Gensler5, Alexander Marten6, Myriam Manente7, George Stojan8, Thomas Vaux9, Katy White9, Atul Deodhar10, Nicola Boffini11, Martin Rudwaleit12 | 1Department of Rheumatology, Radboud University Medical Centre Nijmegen, The Netherlands; 2Genomics England London, United Kingdom; 3Department of Rheumatology, Leiden University Medical Center Leiden, The Netherlands; 4Department of Medicine/Rheumatology, University Health Network, Schroeder Arthritis Institute, University of Toronto Toronto, Canada; 5Department of Medicine/Rheumatology, University of California San Francisco, USA; 6UCB Monheim am Rhein Germany; 7UCB Braine-lAlleud, Belgium; 8UCB Atlanta, USA; 9UCB Slough, United Kingdom; 10Division of Arthritis and Rheumatic Diseases, Oregon Health and Science University Portland, USA; 11IRCCS Ospedale San Raffaele Milan, Italy; 12Klinikum Bielefeld, University of Bielefeld, Bielefeld, Germany
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 18 March 2026
26
Views