62nd National Congress of the Italian Society of Rheumatology
Vol. 77 No. s1 (2025): Abstract book of the 62th Conference of the Italian Society for...
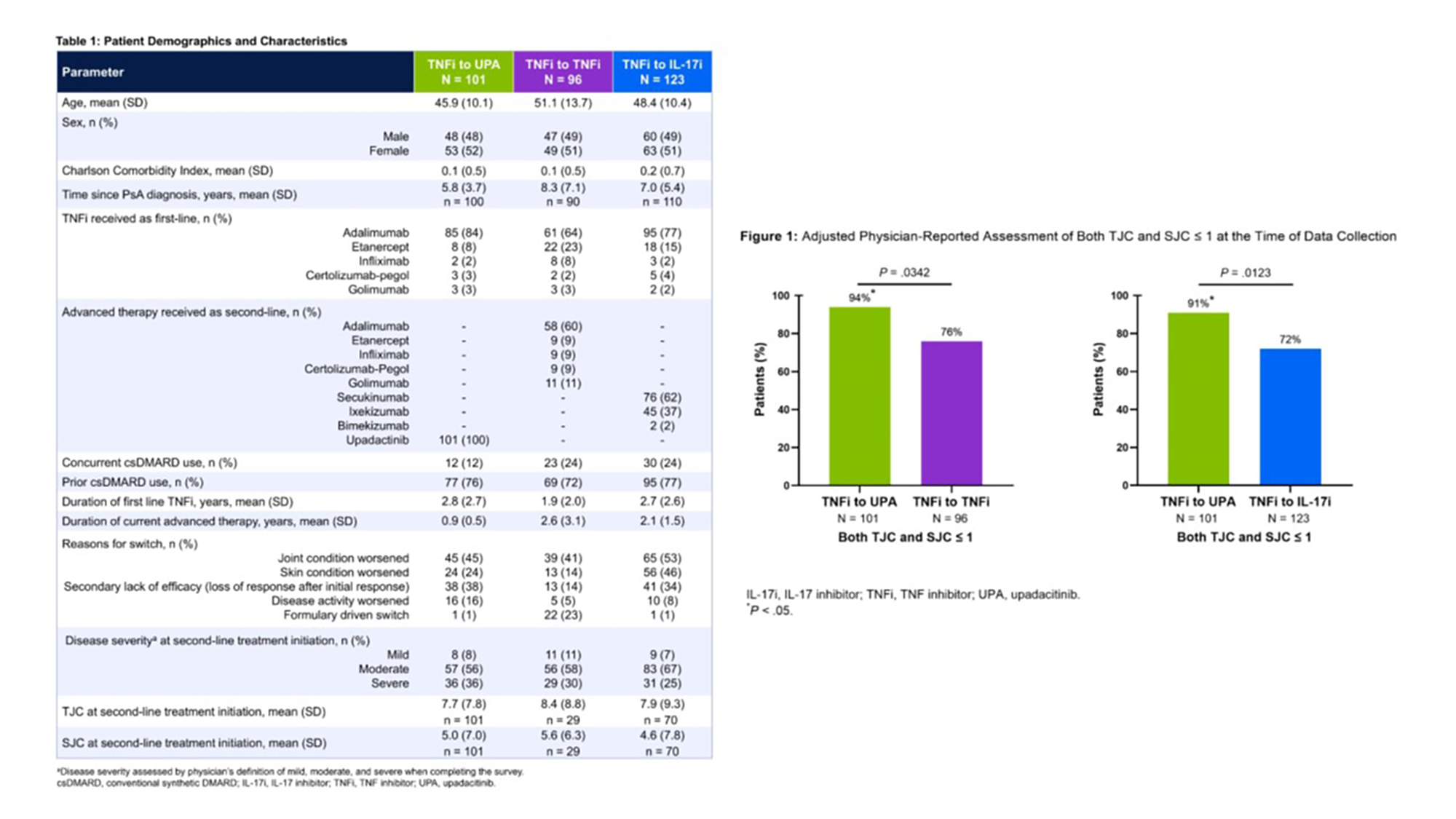
PO:02:025 | Real-World Comparative Effectiveness of Upadacitinib in Psoriatic Arthritis: Evaluation of Switching to Upadacitinib Versus Tumor Necrosis Factor Inhibitors or Interleukin-17 Inhibitors After First-Line Tumor Necrosis Factor Inhibitors
Valentina Carlini1, Philip Mease2, William Tillett3, Xiaolan Ye4, Christopher Saffore4, Molly Edwards5, Isabel Truman5, Sophie Barlow5, Jayne Stigler4, Bhumik Parikh4, Daniel Aletaha6 | 1Abbvie srl Roma, Italy; 2University of Washington School of Medicine Seattle, United States Minor Outlying Islands; 3Department of Rheumatology, Royal National Hospital for Rheumatic Diseases Bath, United Kingdom; 4Abbvie Inc. North Chicago, United States Minor Outlying Islands; 5Adelphi Real World Bollington, United Kingdom; 6Division of Rheumatology, Department of Medicine, Medical University of Vienna, Vienna, Austria
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 18 March 2026
26
Views