62nd National Congress of the Italian Society of Rheumatology
Vol. 77 No. s1 (2025): Abstract book of the 62th Conference of the Italian Society for...
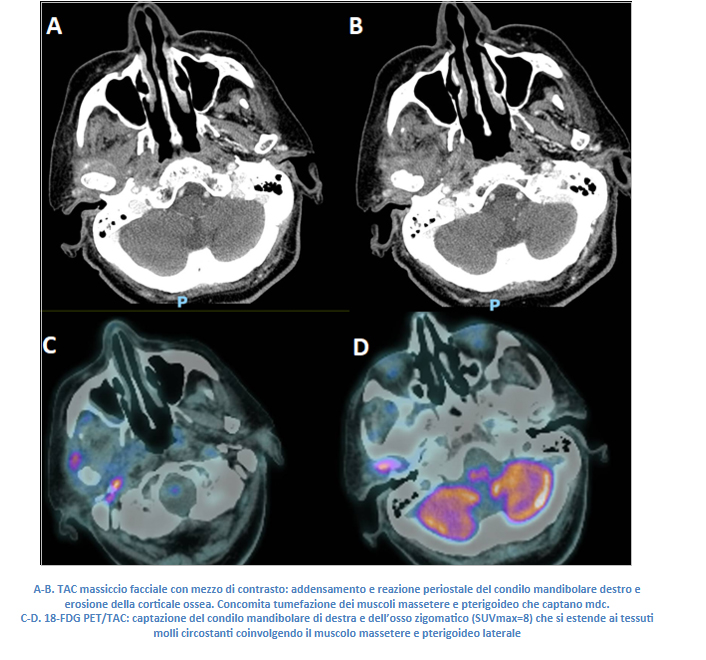
PO:11:158 | Osteomyelitis of the jaw: a rare mimick of giant cell arteritis
Laura Gigante1, Giovanni B. Canestrari1, Olga Addimanda1, Francesca Bergossi1, Angela Buffa1, Francesco Cianci1, Daniela Chiarini1, Niccolò Girolimetto1, Daniele Lini1, Luca Magnani1, Mirco Magnani1, Erika Meleddu1, Francesca Pignataro1, Sofia Testoni1, Alarico Ariani1, Rita Mulè1, Elisa Rossi1, Enrica Vandelli1, Gentiana Vukatana1, Antonella Gamberini1, Massimo Reta1 | 1UO interaziendale Medicina Interna ad Indirizzo Reumatologico - AUSL Bologna - AOSP Sant'Orsola Bologna, Italy
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 25 November 2025
151
Views
Laura Gigante, Giovanni B. Canestrari, Olga Addimanda, Francesca Bergossi, Angela Buffa, Francesco Cianci, Daniela Chiarini, Niccolò Girolimetto, Daniele Lini, Luca Magnani, Mirco Magnani, Erika Meleddu, Francesca Pignataro, Sofia Testoni, Alarico Ariani, Rita Mulè, Elisa Rossi, Enrica Vandelli, Gentiana Vukatana, Antonella Gamberini, Massimo Reta