Case Reports
Vol. 69 No. 2 (2017)
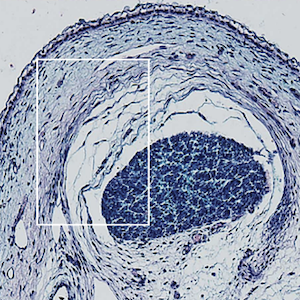
Acute heart failure and rhabdomyolysis: a clue for the diagnosis of polymyositis with cardiac involvement

Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Received: 27 September 2016
Accepted: 27 April 2017
Accepted: 27 April 2017
2317
Views
1039
Downloads